A hypertonic pelvic floor is when the muscles in your pelvic area become really tight and have a hard time stretching. It’s like comparing it to a stress ball. Do you know how some stress balls are really firm and tough to squeeze? Well, the muscles in a hypertonic pelvic floor feel the same way. This condition can have many causes, and it’s actually quite common, but that doesn’t make it any less bothersome. In fact, it can be really uncomfortable and even painful for some people. It’s important to remember that our pelvic floor muscles should be flexible and not feel like a tight stress ball.
As per Continence.org.au :When the muscles in the pelvic floor become really tight and can’t relax properly, it’s called a hypertonic pelvic floor. It can cause a lot of problems with pelvic health. Some common issues that people with a tense pelvic floor experience are constipation (having trouble going to the bathroom), painful sex, always feeling like they need to pee, and pelvic pain.
Sometimes, the tightness in the pelvic floor can also affect other muscles around the hips and pelvis, like the piriformis, obturator internus, coccygeus, and hamstrings. It’s important to address these issues and find ways to help the muscles relax and function properly.
It’s not good when your pelvic floor muscles become tight, tense, and weak because it can affect the blood flow and oxygen supply to those muscles.
Basically, it means that the muscles in your pelvic area aren’t working the way they should, and it can cause some problems.
Hypertonic Pelvic Floor How It Happens?

Here are some of the causes of the hypertonic pelvic floor:
Gynecological causes: Conditions like endometriosis, fibroids, polycystic ovary syndrome (PCOS), pelvic inflammatory disease (PID), and pregnancy.
Genitourinary causes: Interstitial cystitis, cystocele (bladder prolapse), prostatitis (inflammation of the prostate), and sexually transmitted diseases (STDs).
Gastrological causes: Irritable bowel syndrome (IBS), Crohn’s disease, and ulcerative colitis.
Colorectal causes: Hemorrhoids, anal fissures, proctalgia fugax (rectal pain), and a history of colectomy (colon removal surgery).
Neurological causes: Pudendal neuralgia (nerve pain in the pelvic area), migraines, herpes simplex virus (HSV) infection, shingles, and multiple sclerosis (MS).
Rheumatic causes: Conditions like ankylosing spondylitis (inflammatory arthritis affecting the spine), fibromyalgia, and connective tissue disorders with hypermobility.
Musculoskeletal causes: Injuries such as a labral tear in the hip joint, lumbar radiculopathy (pinched nerve in the lower back), and coccyx (tailbone) injury.
Sometimes, the tightness in the pelvic floor muscles can also be related to our emotions and mental well-being.
When we feel anxious, stressed, or have experienced trauma, our muscles can become tense, including the muscles in the pelvic area. So, it’s not just physical factors that can contribute to a hypertonic pelvic floor.
If you suspect that you have a hypertonic pelvic floor, it’s best to seek help from a Pelvic Physical Therapist.
They are experts who can assess your situation and create a personalized treatment plan just for you. Remember, everyone’s case is unique, so it’s important to get the right guidance and support.
Hypertonic Pelvic Floor Symptoms
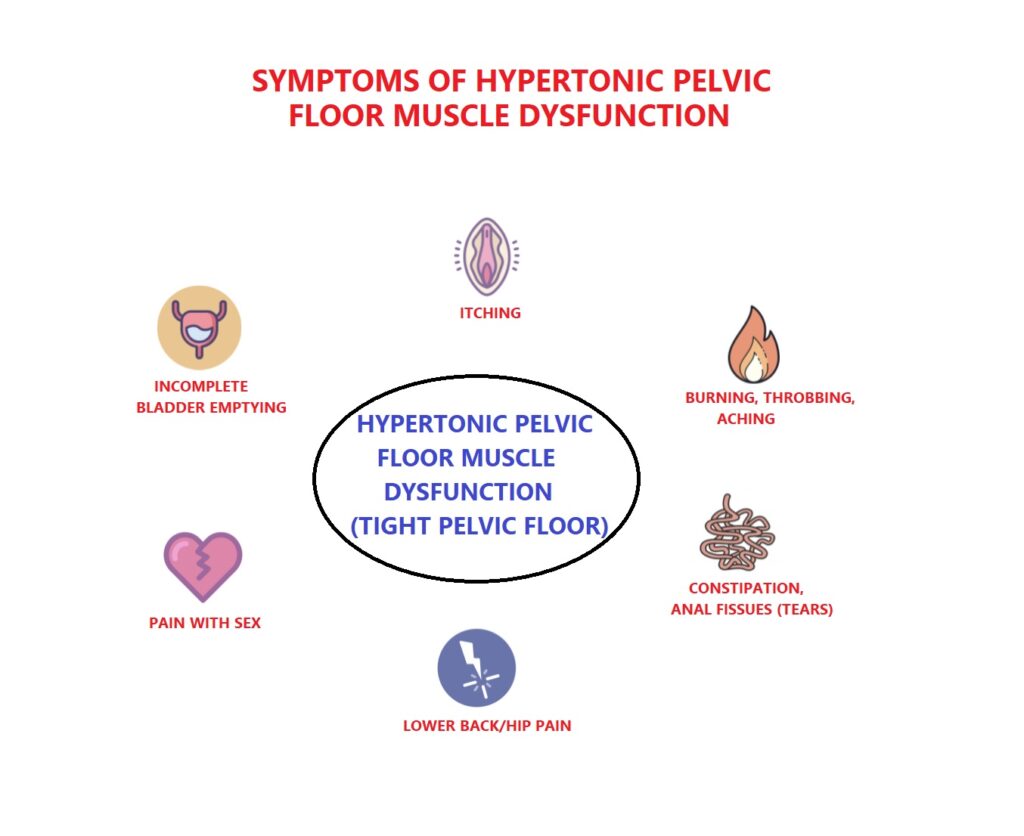
There are many different symptoms that can be associated with a hypertonic pelvic floor. These symptoms can vary from person to person.
If you are feeling such symptoms, then please get an appointment with a Pelvic Physical Therapist.
Here is a list of symptoms commonly associated with a hypertonic pelvic floor:
- Constipation (having difficulty with bowel movements)
- Feeling like your bowels are not completely empty after using the bathroom
- Straining when trying to have a bowel movement
- Pelvic pain
- Low back pain
- Hip pain
- Coccyx (tailbone) pain
- Painful sex
- Vaginismus (involuntary muscle spasms in the vaginal area)
- Urinary incontinence (leaking urine)
- Feeling like your bladder is not completely empty after urinating
- Slow flow of urine
- Hesitancy or delayed start of the urine stream
- Urinary urgency (sudden strong need to urinate)
- Urinary frequency (having to urinate frequently)
- Painful urination
If you experience any of these symptoms, try to pay attention to how they feel when they occur and any patterns you notice.
This information will be helpful to share with your chosen healthcare professional so that they can better understand what might be causing your symptoms.
Hypertonic Pelvic Floor Exercises
Doctors recommend these three exercises to their patients and have noticed amazing results from them. It’s important to perform these exercises slowly and focus on breathing correctly to allow your pelvic floor muscles to fully relax.
There are several pelvic floor yoga poses that can help out in this situation.
Butterfly for hypertonic pelvic floor
This exercise targets the adductor muscles. Sit on the floor and bring the soles of your feet together, allowing your knees to drop out to the sides.
Gently press down on your thighs with your hands to increase the stretch. Hold this position while taking slow, deep breaths.
Squat:
This exercise helps decrease the tension in your pelvic floor muscles. Stand with your feet shoulder-width apart, and slowly lower your body into a squatting position.
Keep your heels on the ground and your back straight. You can place your hands together in front of you for balance. Hold the squat briefly, then slowly rise back up.
Child’s Pose:
This exercise stretches the adductor and glute muscles. Begin by kneeling on the floor and then sit back on your heels.
Slowly lower your upper body forward, reaching your arms out in front of you and resting your forehead on the floor. Take deep breaths and try to relax into the stretch.
Remember to listen to your body and go at your own pace. If any exercise feels uncomfortable or causes pain, stop and consult with a healthcare professional or Pelvic Physical Therapist for guidance.
How to Breath for Hypertonic Pelvic Floor
Breathing techniques can be very beneficial for a hypertonic pelvic floor, and you can easily practice them at home. When performed correctly, these techniques can provide great relief.
Diaphragmatic breathing: This technique involves focusing on breathing deeply into your diaphragm. Start by finding a comfortable position, either sitting or lying down. Put one hand on the chest and another on the abdomen. Breathe in slowly through your nose, allowing your abdomen to rise as you fill your lungs with air. Exhale slowly through your mouth, feeling your abdomen lower. Practice this deep, relaxed breathing for several minutes.
360° breathing: This technique focuses on expanding your breath not just into your abdomen but also into the sides and back of your ribcage. Sit or stand in a comfortable position. Inhale deeply, imagining your breath filling not just your abdomen but also expanding the sides and back of your ribcage. Exhale fully, allowing your breath to release completely. Repeat this pattern, consciously expanding your breath in a 360-degree manner.
Alternate nostril breathing: This technique helps balance the breath and calm the mind. Sit comfortably and bring your right hand up to your face. Use your right thumb to close your right nostril and inhale slowly through your left nostril. Wait for a second, then with your right ring finger, close the left nostril and release the right thumb from the right nostril. Exhale slowly through your right nostril. Inhale with the right nostril, wait for a moment and exhale with the left nostril. Repeat this alternating pattern for several rounds.
Remember to practice these breathing techniques with patience and mindfulness. They can be a valuable addition to your routine for managing a hypertonic pelvic floor. If you have any concerns or specific questions, it’s always a good idea to consult with a healthcare professional or Pelvic Physical Therapist for guidance.
Treatment for Hypertonic Pelvic Floor
Treating a hypertonic pelvic floor involves different approaches to help relax and improve the condition. Here are some common treatments:
Pelvic Physical Therapy
Working with a specialized therapist who focuses on the pelvic area can be really helpful. They will teach you techniques like stretching exercises and biofeedback to relax and retrain your pelvic floor muscles.
Breathing and Relaxation Techniques
Learning specific breathing exercises and relaxation methods can help release tension in the pelvic muscles. These techniques involve deep breathing and mindful relaxation to promote muscle relaxation and reduce pain.
Pelvic Floor Muscle Exercises
Even though the muscles are already tight, targeted exercises can still be beneficial. The focus is on learning to consciously release and lengthen the pelvic floor muscles through specific relaxation exercises.
Education and Lifestyle Changes
Understanding your condition and making some lifestyle adjustments can also make a difference. Improving your posture, avoiding activities that make your symptoms worse, managing stress levels, and eating a healthy diet can all support pelvic health.
Manual Therapy Techniques
Some healthcare professionals, like specialized physical therapists or osteopaths, may use manual therapy techniques to release tightness in surrounding muscles and trigger points that contribute to the hypertonic pelvic floor.
Psychological Support
Stress, anxiety, and emotional factors can affect your pelvic floor muscles. Seeking support from a mental health professional can be helpful. Techniques like talking therapy or mindfulness practices can assist in managing these psychological aspects.
Using Intravaginal Dilator/Wand Therapy for Pelvic Pain
Intravaginal dilator therapy, also known as wand therapy, can be used as a treatment approach for pelvic pain. It involves using specially designed devices, typically called dilators or wands, to gently stretch and desensitize the pelvic floor muscles.
The goal of this therapy is to reduce pelvic muscle tension and improve flexibility. By gradually inserting and using these dilators/wands, individuals can help their muscles become more accustomed to the sensation and promote relaxation.
It’s important to note that intravaginal dilator therapy should be approached under the guidance of a healthcare professional or a Pelvic Physical Therapist. They can provide instructions on the proper technique and appropriate sizes of dilators/wands to use and help create a personalized treatment plan based on individual needs.
It’s always recommended to consult with a healthcare professional before starting any new treatment to ensure it is suitable for your specific condition and to receive proper guidance throughout the process.
Recommendation
What is an Innie and Outie Vagina?
What’s the Best Time of Day to Do Yoga?




